Why Seniors Shouldn’t Ignore These Atopic Dermatitis Signs
Atopic dermatitis, also known as eczema, is a chronic skin condition that can affect individuals of all ages, including seniors. While it’s commonly associated with younger populations, older adults are also at risk of developing or worsening symptoms. It’s important for seniors to recognize the signs of atopic dermatitis early to prevent complications and improve quality of life. Understanding these key symptoms and taking proactive steps can help manage the condition and minimize its impact.
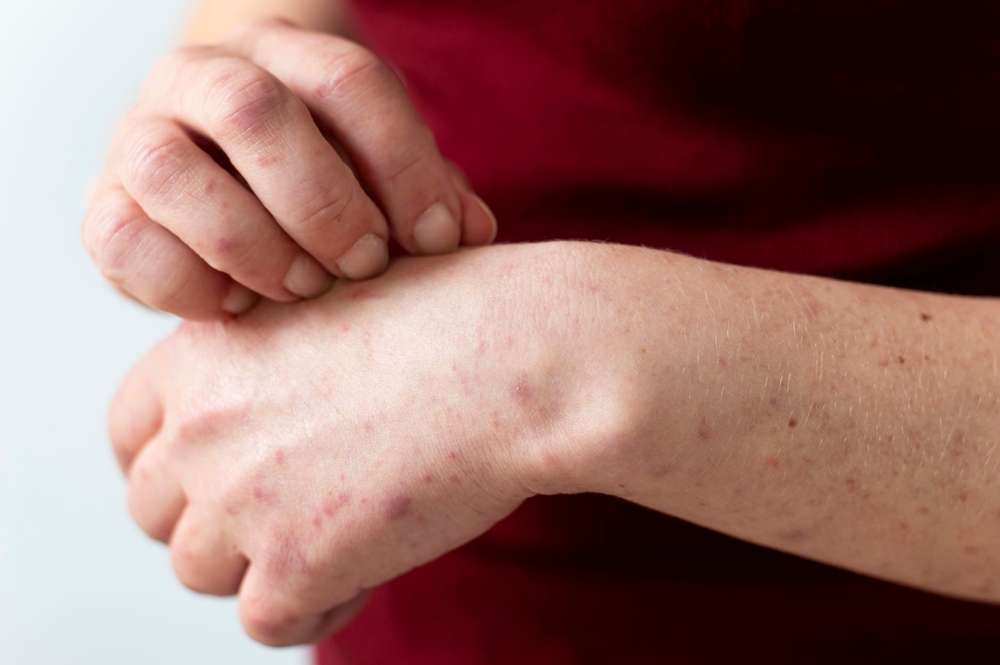
Aging skin naturally becomes thinner, drier, and more fragile, which can make rashes easier to miss—or easy to dismiss as “just dry skin.” But when itching and inflammation become persistent, widespread, or repeatedly flare, it can point to atopic dermatitis. In older adults, paying attention to pattern, severity, and complications matters because untreated skin inflammation can affect comfort, sleep, and overall day-to-day functioning.
What Is Atopic Dermatitis and How Does It Affect Seniors?
Atopic dermatitis is a chronic inflammatory skin condition that often causes itching, redness, and a weakened skin barrier. While many people associate it with childhood eczema, it can persist into later life or appear for the first time in older adulthood. In seniors, reduced oil production, slower skin repair, and more frequent exposure to irritants (such as frequent handwashing or medical adhesives) can make symptoms more noticeable and harder to control.
It is also common for atopic dermatitis to overlap with other issues that are more prevalent with age, such as dry skin (xerosis), venous stasis dermatitis in the lower legs, or medication-related rashes. Because these conditions can look similar, persistent or worsening symptoms deserve a careful evaluation rather than repeated trial-and-error with over-the-counter products.
What Are the Common Signs of Atopic Dermatitis in Older Adults?
In seniors, the hallmark symptom is often intense itching that may worsen at night. Skin may look red, scaly, rough, or thickened from chronic scratching, and it can feel tight or painful—especially after bathing. Commonly affected areas include the hands, arms, trunk, and legs; some older adults also develop patches on the face or neck.
Warning signs that should not be ignored include cracking, oozing, crusting, or open sores, which can raise concern for secondary infection. Another clue is a pattern of flares: symptoms improve briefly and then return, particularly after exposure to certain soaps, fabrics, or environmental changes. If a rash appears suddenly, spreads rapidly, forms blisters, or is accompanied by fever or significant swelling, it warrants prompt medical assessment.
How Does Atopic Dermatitis Impact Senior Health and Well-being?
Persistent itch and discomfort can disrupt sleep, which may contribute to fatigue, irritability, and reduced resilience during the day. Broken skin from scratching can create entry points for bacteria, increasing the likelihood of skin infections that may require prescription treatment. For seniors with diabetes, poor circulation, or immune compromise, skin infections and delayed healing can be especially concerning.
Atopic dermatitis can also affect daily routines. Dressing may become uncomfortable, bathing may sting, and some people avoid social activities due to visible rashes. Caregivers may notice increased agitation, repetitive scratching, or reluctance to allow skin care—signs that symptoms are affecting quality of life. When managed consistently, however, many seniors experience fewer flares and better comfort.
What Are the Common Triggers for Atopic Dermatitis in Seniors?
Triggers vary, but many relate to dryness and irritation. Hot showers, long baths, harsh soaps, fragranced products, and frequent hand sanitizers can strip the skin barrier. Low indoor humidity during winter, heat exposure in summer, and friction from rough fabrics can also contribute to flares. Some seniors react to topical products they previously tolerated, especially those containing fragrances, preservatives, or certain botanical ingredients.
Medical and lifestyle factors may play a role as well. Stress can worsen itch and inflammation. Some medications can cause rashes that mimic eczema or can dry the skin, complicating symptom control. In addition, underlying conditions that affect circulation or swelling in the legs may change skin integrity and make lower-leg dermatitis harder to manage. Keeping a simple symptom diary—what was used on the skin, bathing habits, weather changes, and flare timing—can help identify patterns.
What Treatment and Management Options Are Available for Seniors?
Management typically focuses on restoring the skin barrier, reducing inflammation, and preventing infection. Daily moisturizing is often the foundation: thick, fragrance-free creams or ointments applied within minutes after bathing can reduce dryness and itch. Gentle cleansing with mild, fragrance-free products and lukewarm water helps limit irritation. For localized inflammation, clinicians may recommend topical anti-inflammatory medications (such as corticosteroids or non-steroidal prescription creams), selected carefully to match skin sensitivity and the body area being treated.
When symptoms are widespread, severe, or not improving, a clinician may consider additional options such as phototherapy or systemic medications, balancing benefits with other health conditions and potential side effects. Seniors should also ask about safer itch-control strategies—like targeted moisturizers, wet wrap approaches when appropriate, or antihistamines only when clinically suitable—because some sedating medications can increase fall risk. Regular follow-up is important if flares are frequent, if infection is suspected, or if the diagnosis is uncertain.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.
A practical approach for many older adults is to treat skin care like a routine: brief lukewarm showers, immediate moisturization, and consistent avoidance of known irritants. When symptoms persist despite these steps—or when there is cracking, oozing, significant pain, or sleep disruption—evaluation by a clinician (often a primary care provider or dermatologist) can help confirm the cause and tailor treatment to aging skin. Recognizing early signs and addressing them steadily can reduce flares and support comfort over time.






