Understanding Plaque Psoriasis: Key Signs That Indicate a Potential Problem
Plaque psoriasis is a chronic autoimmune condition that causes the rapid buildup of skin cells, leading to thick, scaly patches on the skin. These plaques can be itchy, painful, and emotionally distressing. While it’s not contagious, psoriasis can significantly affect a person’s quality of life if left unmanaged. Recognizing the early signs of plaque psoriasis is essential for timely treatment and long-term skin health. Awareness of its symptoms can help reduce flare-ups and discomfort.
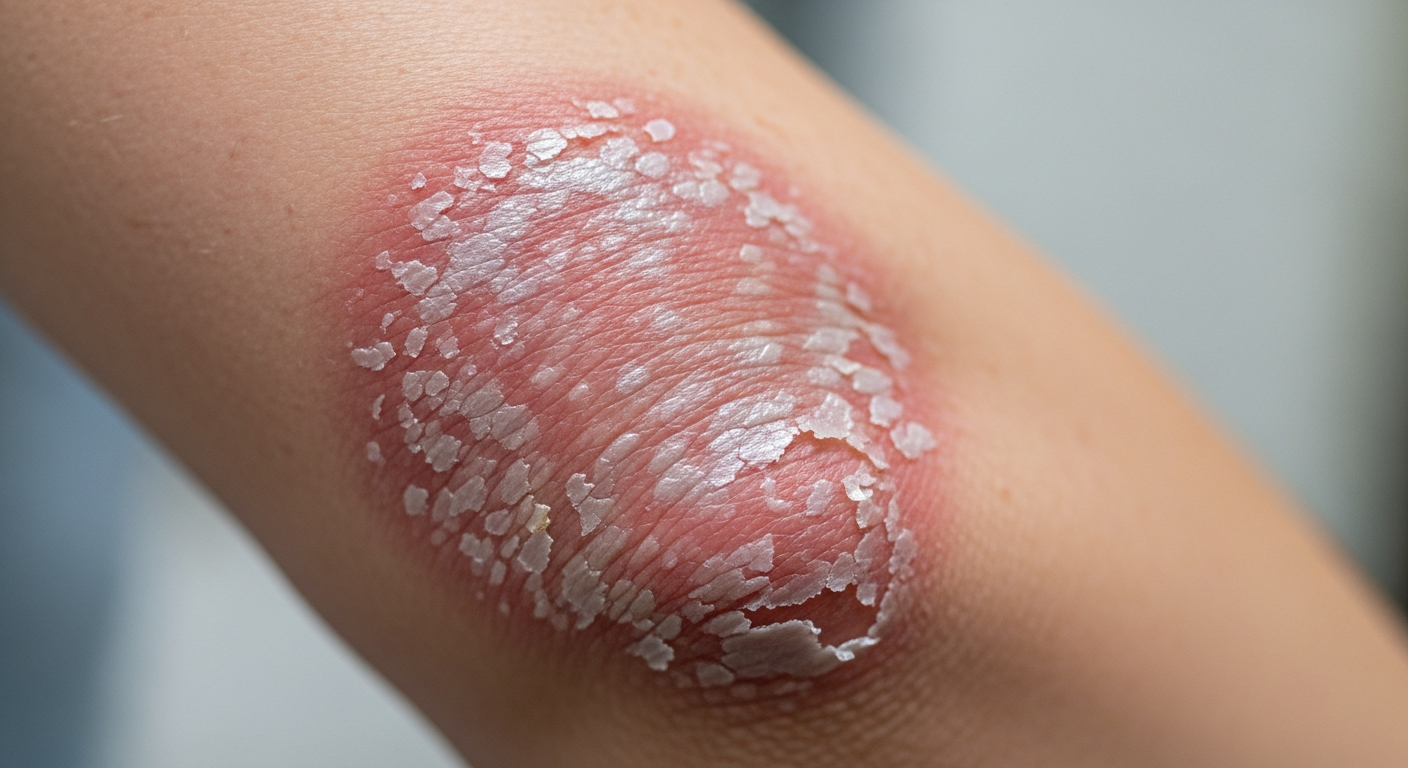
Skin symptoms can look similar across many conditions, but plaque psoriasis often follows recognizable patterns in texture, color, location, and day-to-day irritation. Paying attention to those patterns can help you track changes over time and communicate what you’re experiencing more accurately during a medical visit. It can also reduce guesswork when deciding whether a flare is improving, staying the same, or worsening.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.
What are scaly patches in plaque psoriasis?
Scaly patches are one of the most recognizable signs of plaque psoriasis. They typically appear as well-defined, raised areas of skin covered by a buildup of dry, silvery-white scale. This scaling happens when skin cells turn over faster than usual, leading to accumulation on the surface. The plaques may crack, feel tight, or shed flakes—sometimes resembling dandruff when they occur on the scalp.
A helpful clue is persistence: plaques often last for weeks or months and may return in the same spots. Another clue is the edge of the plaque, which is often clearly demarcated compared with surrounding skin. While dryness alone can improve quickly with moisturizers, psoriasis plaques often require targeted management to calm inflammation and slow excessive skin cell growth.
How do itching and burning symptoms show up?
Itching can range from mild to intense and may come and go with flares. Some people describe a deep itch that is hard to relieve, while others notice stinging, burning, or soreness—especially in areas where skin rubs against clothing or where plaques crack. Scratching can damage the skin barrier, increase irritation, and raise the chance of bleeding or secondary infection.
Burning sensations can be linked to active inflammation, fissures (small splits in the skin), or sensitivity from frequent washing and harsh products. Tracking when itching or burning worsens—after hot showers, stress, alcohol use, or certain weather conditions—can reveal patterns that support better symptom management. If discomfort is severe, disrupts sleep, or is paired with warmth, swelling, or oozing, it’s important to seek clinical advice.
Why monitor redness and visible inflammation?
Redness in plaque psoriasis reflects inflammation in the skin. Depending on skin tone, inflammation may look bright pink, red, purple, or dark brown, and it may be easier to feel than see—such as warmth, tenderness, or thickening. Monitoring redness matters because it can signal whether a plaque is actively inflamed, spreading, or calming down.
A practical approach is to note changes in three features: color intensity, thickness, and scaling. For example, scaling may decrease while redness remains, or redness may fade but thickness persists. Photographs taken in consistent lighting can help you detect gradual changes that are easy to miss day-to-day. If redness rapidly expands, becomes very painful, or is accompanied by fever or pus, prompt medical assessment is warranted because other skin problems can overlap or mimic psoriasis.
How can plaque location help identify the condition?
Location can provide useful clues because plaque psoriasis commonly affects specific areas. Typical sites include the elbows, knees, scalp, lower back, and the area around the belly button. Plaques often occur symmetrically (for example, both elbows) and may develop where the skin experiences friction or minor injury. This phenomenon—new lesions appearing at sites of scratching, rubbing, or cuts—is sometimes called the Koebner response.
Psoriasis can also involve nails, leading to pitting (small dents), thickening, crumbling, or separation from the nail bed. Nail changes can be an important sign, especially when skin plaques are subtle. In skin folds (under breasts, groin, armpits), psoriasis may look smoother and less scaly because moisture reduces visible flaking, which can make it harder to recognize without considering the overall pattern.
What treatment options are used for plaque psoriasis?
Treatment is usually tailored to severity, location, and how much the condition affects daily life. For mild to moderate disease, clinicians often start with topical therapies that reduce inflammation and scaling, such as corticosteroid creams/ointments, vitamin D analogs, retinoids, or combination products. Regular use of bland moisturizers can support the skin barrier and reduce cracking and discomfort, even when prescription treatments are needed.
For more extensive or resistant psoriasis, phototherapy (controlled exposure to specific ultraviolet light) may be considered. Systemic treatments—oral medications or injectable biologic therapies—can be used when psoriasis is widespread, significantly symptomatic, or associated with complications. Because psoriasis is an immune-mediated condition, some systemic options require lab monitoring and screening for infections.
It’s also important to watch for joint symptoms such as morning stiffness, swelling, or pain in fingers, toes, or the lower back, which can suggest psoriatic arthritis and may change the treatment approach. A clinician can help confirm the diagnosis, rule out look-alike conditions, and select a plan that balances effectiveness and safety.
In summary, plaque psoriasis commonly presents with persistent, well-defined scaly patches, varying degrees of itch or burning, and visible (or palpable) inflammation that may recur in characteristic locations like elbows, knees, and scalp. Noticing details such as symmetry, plaque thickness, triggers, and nail changes can make symptom tracking more meaningful. With an accurate diagnosis, treatment can be matched to the severity and location of disease, supporting steadier control over flares and day-to-day comfort.






